A Comparative Study of QCT and DXA on Detection of Osteoporosis in Postmenopausal Women
-
摘要:
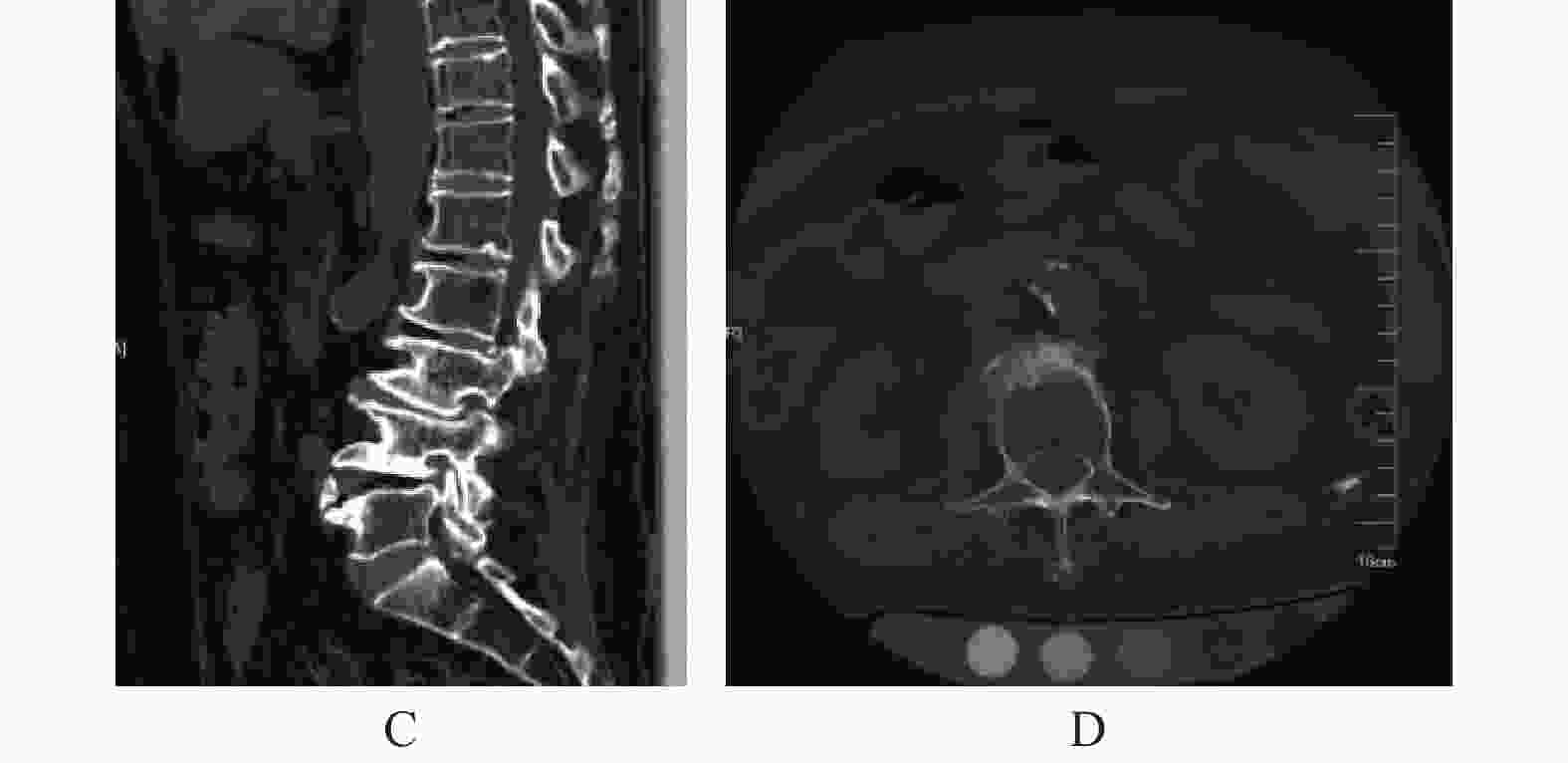
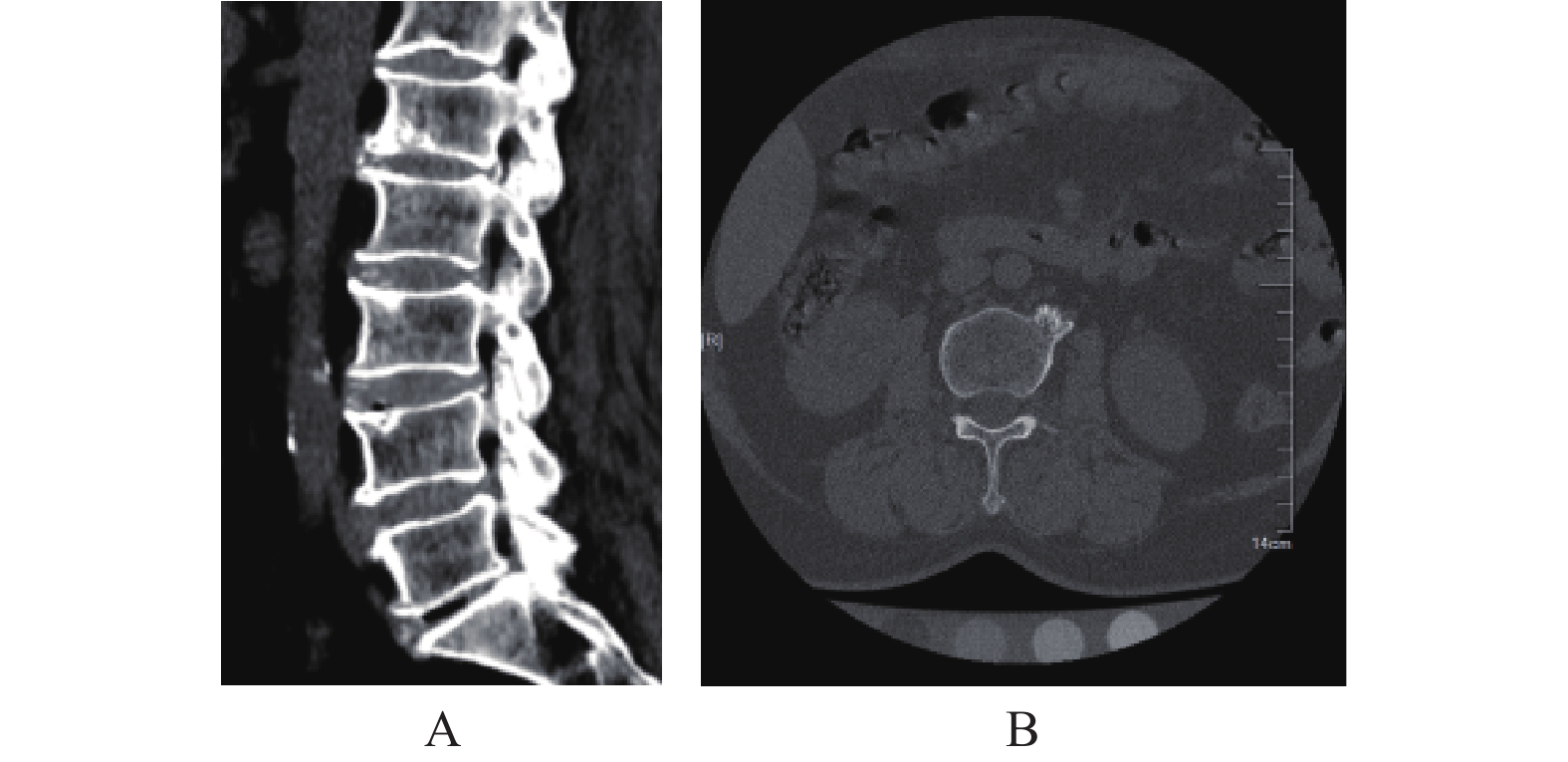
目的 对比定量计算机断层扫描法(quantitative computed tomography,QCT)与双能 X 线吸收法( dual energy X-ray absorptiometry,DXA)在绝经后妇女中骨质疏松症的检出率,并分析两者差异性的原因。 方法 收集的148例绝经后妇女,平均年龄(63.7±10.4)岁,分别采用DXA、QCT测量腰椎骨密度(bone mineral density,BMD),计算2种方法对骨质疏松症的检出率,并对测量的结果进行分析比较,查看诊断不一致患者的腰椎CT平扫图像,以评估是否有椎体骨折、脊柱退行性改变和腹主动脉钙化等情况。 结果 148例受试者,QCT的检出率为45.9%(68/148),DXA的检出率为26.4%(39/148),差异有统计学意义(P < 0.05)。92例受试者(62.2%)的DXA和QCT的诊断是一致的;56例(37.8%)受试者DXA和QCT的诊断不一致,其中QCT诊断为骨质疏松,DXA为骨量减少的例数占48.2%(27/56);QCT为骨量减少,DXA为骨量正常的例数占33.9%(19/56)。在56例诊断不一致的患者中2例(2/56)为椎体压缩骨折,56例(56/56)均有腰椎退行性变(骨赘、终板硬化、韧带骨化或小关节骨关节炎),9例(9/56)有腹主动脉钙化。 结论 QCT与DXA对骨质疏松症的检出率不一致,这可能是由于患者存在脊柱退行性变、腹主动脉钙化和其他硬化性病变等情况,这会使DXA测得的BMD值升高,导致DXA检出率降低。相比于DXA,QCT是诊断绝经后妇女骨质疏松症一种更敏感的方法。 -
关键词:
- 绝经后妇女 /
- 骨质疏松症 /
- 双能 X 线吸收法 /
- 定量计算机断层扫描法 /
- 骨密度
Abstract:Objective To compare the detection rate of osteoporosis in postmenopausal women with quantitative computed tomography (QCT) and dual energy X-ray absorptiometry (DXA), and analyze the causes for differences. Methods A total of 148 postmenopausal women were enrolled, with an average age of (63.7±10.4) years old. The lumbar spine bone mineral density was measured by DXA and QCT, respectively. The detection rate of osteoporosis by the two methods was calculated, and the measurement results were analyzed and compared. The plain CT images of patients with inconsistent diagnosis were checked to evaluate whether there were vertebral fracture, degenerative changes of spine and aorta abdominalis calcification. Results In 148 subjects, the detection rate of QCT was 45.9% (68/148), and the detection rate of DXA was 26.4% (39/148), the difference was statistically significant (P < 0.05). The diagnosis of DXA and QCT was consistent in 92 subjects (62.2%); the diagnosis of DXA and QCT was inconsistent in 56 subjects (37.8%). 48.2% of the patients (27/56) were diagnosed as osteoporosis by QCT and bone mass reduction by DXA. 33.9% (19/56) of patients were diagnosed as bone mass reduction by QCT and normal bone mass by DXA. Of all patients with inconsistent diagnosis, 2 (2/56) had vertebral compression fractures, and 56 (56/56) had lumbar degeneration (osteophytes, endplate sclerosis, ligament ossification or facet joint osteoarthritis), 9 (9/56) had abdominal aortic calcification. Conclusion The inconsistent detection rates of osteoporosis between QCT and DXA may be caused by the presence of spinal degeneration, abdominal aortic calcification and other sclerotic lesions, which will increase the BMD value of DXA, resulting in the higher detection rate of QCT than DXA. Compared with DXA, QCT is a more sensitive method for the diagnosis of osteoporosis in postmenopausal women. -
表 1 QCT与DXA对骨质疏松检出率的比较[n(%)]
Table 1. Comparison of the detection rate of osteoporosis between QCT and DXA [n(%)]
项目 DXA 骨量正常 骨量减少 骨质疏松 总计 QCT 骨量正常 35(23.6) 2(1.4) 1(0.7) 38(25.7) 骨量减少 19(12.8) 21(14.2) 2(1.4) 42(28.4) 骨质疏松 5(3.4) 27(18.2) 36(24.3) 68(45.9) 总计 59(39.9) 50(33.8) 39(26.4) 148(100) McNemar-Bowker Test 37.980 P 0.000* *P < 0.05。 -
[1] Peck W A,Burckhardt P,Christiansen C,et al. Consensus development conference:Diagnosis,prophylaxis,and treatment of osteoporosis[J]. Am J Med,1993,94(6):646-650. doi: 10.1016/0002-9343(93)90218-E [2] 夏维波,章振林,林华,等. 原发性骨质疏松症诊疗指南(2017)[J]. 中国骨质疏松杂志,2019,25(3):281-309. doi: 10.3969/j.issn.1006-7108.2019.03.001 [3] Wade S W,Strader C,Fitzpatrick L A,et al. Estimating prevalence of osteoporosis:Examples from industrialized countries[J]. Arch Osteoporos,2014,9(1):182. doi: 10.1007/s11657-014-0182-3 [4] Seo S H,Lee J,Park I H. Efficacy of dual energy X-ray absorptiometry for evaluation of biomechanical properties:Bone mineral density and actual bone strength[J]. J Bone Metab,2014,21(3):205-212. doi: 10.11005/jbm.2014.21.3.205 [5] Fang Y,Li W,Chen X,et al. Opportunistic osteoporosis screening in multi-detector CT images using deep convolutional neural networks[J]. Eur Radiol,2021,31(4):1831-1842. doi: 10.1007/s00330-020-07312-8 [6] Genant H K,Engelke K,Fuerst T,et al. Noninvasive assessment of bone mineral and structure:State of the art[J]. J BoneMiner Res,1996,11(6):707-730. [7] Blake GM,Fogelman I. Technical principles of dual energy X-ray absorptiometry[J]. Semin Nucl Med,1997,27(3):210e228. [8] Zeng Q, Li N, Wang Q, et al. The prevalence of osteoporosis in China, a nationwide, multicenter DXA survey[J]. J Bone Miner Res, 2019 , 34(10): 1789-1797. [9] Wang P,She W,Mao Z,et al. Use of routine computed tomography scans for detecting osteoporosis in thoracolumbar vertebral bodies[J]. Skeletal Radiol,2021,50(2):371-379. doi: 10.1007/s00256-020-03573-y [10] Mao S S,Li D,Syed Y S,et al. Thoracic quantitative computed tomography (QCT) can sensitively monitor bone mineral metabolism:Comparison of thoracic QCT vs lumbar QCT and dual-energy X-ray absorptiometry in detection of age-relative change in bone mineral density[J]. Acad Radiol,2017,24(12):1582-1587. doi: 10.1016/j.acra.2017.06.013 [11] Salzmann S N,Okano I,Jones C,et al. Thoracic bone mineral density measured by quantitative computed tomography in patients undergoing spine surgery[J]. Spine J,2021,21(11):1866-1872. doi: 10.1016/j.spinee.2021.05.016 [12] Yuan Y,Zhang P,Tian W,et al. Application of bone turnover markers and DXA and QCT in an elderly Chinese male population[J]. Ann Palliat Med,2021,10(6):6351-6358. doi: 10.21037/apm-21-612 [13] Amstrup A K,Jakobsen N F,Moser E,et al. Association between bone indices assessed by DXA,HR-pQCT and QCT scans in post-menopausal women[J]. J Bone Miner Metab,2016,34(6):638-645. doi: 10.1007/s00774-015-0708-9 [14] Link T M. Osteoporosis imaging:State of the art and advanced imaging[J]. Radiology,2012,263(1):3-17. doi: 10.1148/radiol.12110462 [15] López Picazo M,Humbert L,Di Gregorio S,et al. Discrimination of osteoporosis-related vertebral fractures by DXA-derived 3D measurements:A retrospective case-control study[J]. Osteoporos Int,2019,30(5):1099-1110. doi: 10.1007/s00198-019-04894-y [16] Genant H K,Engelke K,Hanley D A,et al. Denosumab improves density and strength parameters as measured by QCT of the radius in postmenopausal women with low bone mineral density[J]. Bone,2010,47(1):131-139. doi: 10.1016/j.bone.2010.04.594 [17] Löffler M T,Jacob A,Valentinitsch A,et al. Improved prediction of incident vertebral fractures using opportunistic QCT compared to DXA[J]. Eur Radiol,2019,29(9):4980-4989. doi: 10.1007/s00330-019-06018-w [18] Shuhart C R,Yeap S S,Anderson P A,et al. Executive summary of the 2019 ISCD position development conference on monitoring treatment,DXA cross-calibration and Least significant change,spinal cord injury,peri-prosthetic and orthopedic bone health,transgender medicine,and pediatrics[J]. Journal of Clinical Densitometry,2019,22(4):453-471. doi: 10.1016/j.jocd.2019.07.001 [19] Johannesdottir F,Allaire B,Kopperdahl D L,et al. Bone density and strength from thoracic and lumbar CT scans both predict incident vertebral fractures independently of fracture location[J]. Osteoporos Int,2021,32(2):261-269. doi: 10.1007/s00198-020-05528-4 [20] Pickhardt P J,Pooler B D,Lauder T,et al. Opportunistic screening for osteoporosis using abdominal computed tomography scans obtained for other indications[J]. Ann Intern Med,2013,158(8):588-595. doi: 10.7326/0003-4819-158-8-201304160-00003 [21] 程晓光,李娜,余卫. 美国放射学院(ACR)关于定量CT(QCT)骨密度测量操作指南[J]. 中国骨质疏松杂志,2013,19(9):991-997. doi: 10.3969/j.issn.1006-7108.2013.09.026 [22] Tothill P,Hannan W J,Cowen S,et al. Anomalies in the measurement of changes in total-body bone mineral by dual-energy X-ray absorptiometry during weight change[J]. J Bone Miner Res,1997,12(11):1908-1921. doi: 10.1359/jbmr.1997.12.11.1908 [23] Link T M,Lang T F. Axial QCT:Clinical applications and new developments[J]. J Clin Densitom,2014,17(4):438-448. doi: 10.1016/j.jocd.2014.04.119 [24] Okano I,Salzmann S N,Jones C,et al. The impact of degenerative disc disease on regional volumetric bone mineral density (vBMD) measured by quantitative computed tomography[J]. Spine,2020,20(2):181-190. doi: 10.1016/j.spinee.2019.02.017 [25] Geng J,Wang L,Li Q,et al. The association of lumbar disc herniation with lumbar volumetric bone mineral density in a cross-sectional chinese study[J]. Diagnostics (Basel),2021,11(6):938. doi: 10.3390/diagnostics11060938 [26] Paggiosi M A,Debono M,Walsh J S,et al. Quantitative computed tomography discriminates between postmenopausal women with low spine bone mineral density with vertebral fractures and those with low spine bone mineral density only:The SHATTER study[J]. Osteoporos Int,2020,31(4):667-675. doi: 10.1007/s00198-020-05317-z [27] Gehweiler D,Schultz M,Schulze M,et al. Material properties of human vertebral trabecular bone under compression can be predicted based on quantitative computed tomography[J]. BMC Musculoskelet Disord,2021,22(1):709. doi: 10.1186/s12891-021-04571-4 [28] Hsu Y,Hsieh T J,Ho C H,et al. Effect of compression fracture on trabecular bone score at lumbar spine[J]. Osteoporos Int,2021,32(5):961-970. doi: 10.1007/s00198-020-05707-3 [29] Wang X,Sanyal A,Cawthon P M,et al. Prediction of new clinical vertebral fractures in elderly men using finite element analysis of CT scans[J]. J Bone MinerRes,2012,27(4):808-816. doi: 10.1002/jbmr.1539 [30] Greenspan S L,Von Stetten E,Emond S K,et al. Instant vertebral assessment:A noninvasive dual X-ray absorptiometry technique to avoid misclassification and clinical mismanagement of osteoporosis[J]. J Clin Densitom,2001,4(4):373-380. doi: 10.1385/JCD:4:4:373 [31] Lee S J,Binkley N,Lubner M G,et al. Opportunistic screening for osteoporosis using the sagittal reconstruction from routine abdominal CT for combined assessment of vertebral fractures and density[J]. Osteoporos Int,2016,27(3):1131-1136. doi: 10.1007/s00198-015-3318-4 [32] Löffler M T,Jacob A,Scharr A,et al. Automatic opportunistic osteoporosis screening in routine CT:Improved prediction of patients with prevalent vertebral fractures compared to DXA[J]. Eur Radiol,2021,31(8):6069-6077. doi: 10.1007/s00330-020-07655-2 [33] Marinova M,Edon B,Wolter K,et al. Use of routine thoracic and abdominal computed tomography scans for assessing bone mineral density and detecting osteoporosis[J]. Curr Med Res Opin,2015,31(10):1871-81. doi: 10.1185/03007995.2015.1074892 [34] Amstrup A K,Jakobsen N F,Lomholt S,et al. Inverse correlation at the hip between areal bone mineral density measured by dual-energy X-ray absorptiometry and cortical volumetric bone mineral density measured by quantitative computed tomography[J]. J Clin Densitom,2016,19(2):226-33. doi: 10.1016/j.jocd.2015.01.002 [35] Anderson K B, Holloway-Kew K L, Mohebbi M, et al. Is trabecular bone score less affected by degenerative-changes at the spine than lumbar spine BMD[J] Arch Osteoporos, 2018 , 13(1): 127. [36] Rajan R,Cherian K E,Kapoor N,et al. Trabecular bone score-an emerging tool in the management of osteoporosis[J]. Indian J Endocrinol Metab,2020,24(3):237-243. doi: 10.4103/ijem.IJEM_147_20 [37] Tenne M,McGuigan F,Besjakov J,et al. Degenerative changes at the lumbar spine-implications for bone mineral density measurement in elderly women[J]. Osteoporos Int,2013,24(4):1419-1428. doi: 10.1007/s00198-012-2048-0 [38] Kim Y W,Kim J H,Yoon S H,et al. Vertebral bone attenuation on low-dose chest CT:Quantitative volumetric analysis for bone fragility assessment[J]. Osteoporos Int,2017,28(1):329-338. doi: 10.1007/s00198-016-3724-2 [39] Carlson B B,Salzmann S N,Shirahata T,et al. Prevalence of osteoporosis and osteopenia diagnosed using quantitative CT in 296 consecutive lumbar fusion patients[J]. Neurosurg Focus,2020,49(2):5. doi: 10.3171/2020.5.FOCUS20241 [40] Adams J E. Quantitative computed tomography[J]. Eur J Radiol,2009,71(3):425-424. doi: 10.1016/j.ejrad.2008.04.060 [41] Cherukuri L, Kinninger A, Birudaraju D, et al. Effect of body mass index on bone mineral density is age-specific. [J] Nutr Metab Cardiovasc Dis, 2021, 31(6): 1767-1773. [42] Löffler M T,Sollmann N,Mei K,et al. X-ray-based quantitative osteoporosis imaging at the spine[J]. Osteoporos Int,2020,31(2):233-250. doi: 10.1007/s00198-019-05212-2 [43] Cheng X,Zhao K,Zha X,et al. China health big data (China biobank) project investigators. Opportunistic screening using low-dose CT and the prevalence of osteoporosis in China:A nationwide,multicenter study[J]. J Bone Miner Res,2021,36(3):427-435. doi: 10.1002/jbmr.4187 [44] Pan Y,Shi D,Wang H,et al. Automatic opportunistic osteoporosis screening using low-dose chest computed tomography scans obtained for lung cancer screening[J]. Eur Radiol,2020,30(7):4107-4116. doi: 10.1007/s00330-020-06679-y [45] Varney E,Abou Elkassem A,Khan M,et al. Prospective validation of a rapid CT-based bone mineral density screening method using colored spinal images[J]. Abdom Radiol (NY),2021,46(4):1752-1760. doi: 10.1007/s00261-020-02791-1 [46] Yasaka K,Akai H,Kunimatsu A,et al. Prediction of bone mineral density from computed tomography:Application of deep learning with a convolutional neural network[J]. Eur Radiol,2020,30(6):3549-3557. doi: 10.1007/s00330-020-06677-0 [47] Padlina I,Gonzalez-Rodriguez E,Hans D,et al. The lumbar spine age-related degenerative disease influences the BMD not the TBS:The Osteolaus cohort[J]. Osteoporos Int,2017,28(3):909-915. doi: 10.1007/s00198-016-3829-7 [48] Deng G,Yin L,Li K,et al. Relationships between anthropometric adiposity indexes and bone mineral density in a cross-sectional Chinese study[J]. Spine J,2021,21(2):332-342. doi: 10.1016/j.spinee.2020.10.019 [49] Alacreu E,Moratal D,Arana E. Opportunistic screening for osteoporosis by routine CT in Southern Europe[J]. Osteoporos Int,2017,28(3):983-990. doi: 10.1007/s00198-016-3804-3 -






 下载:
下载: