Influencing Factors of First-episode Adolescent Depression with Suicidal Ideation in A Minority Ethnic Concentrated Region in Southern Yunnan
-
摘要:
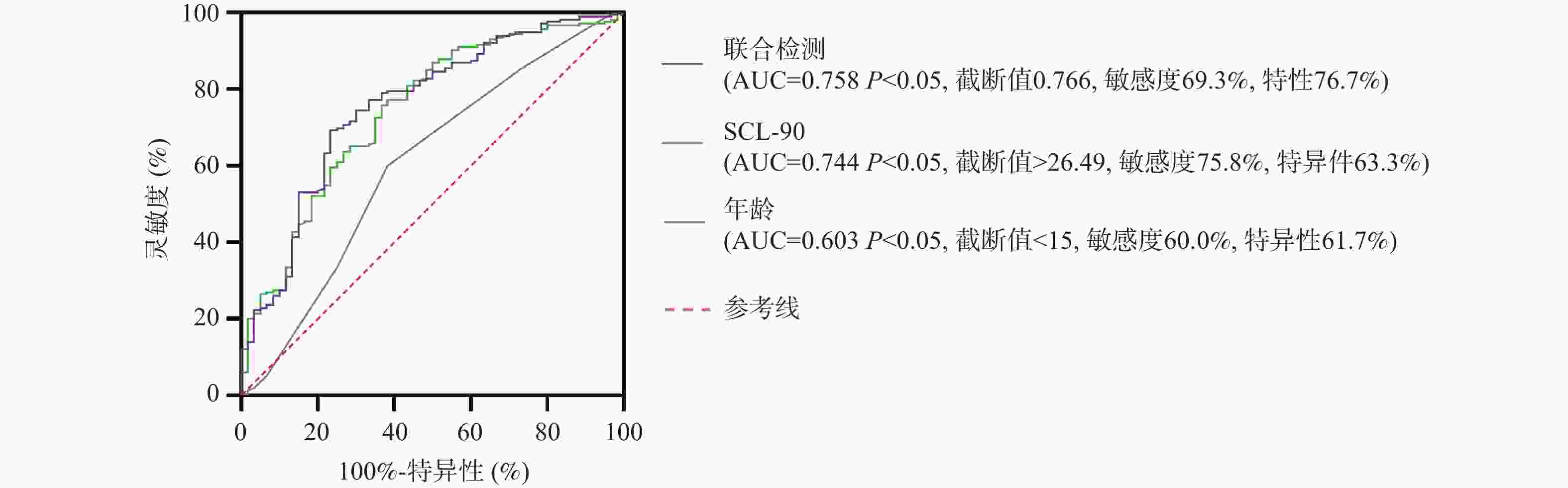
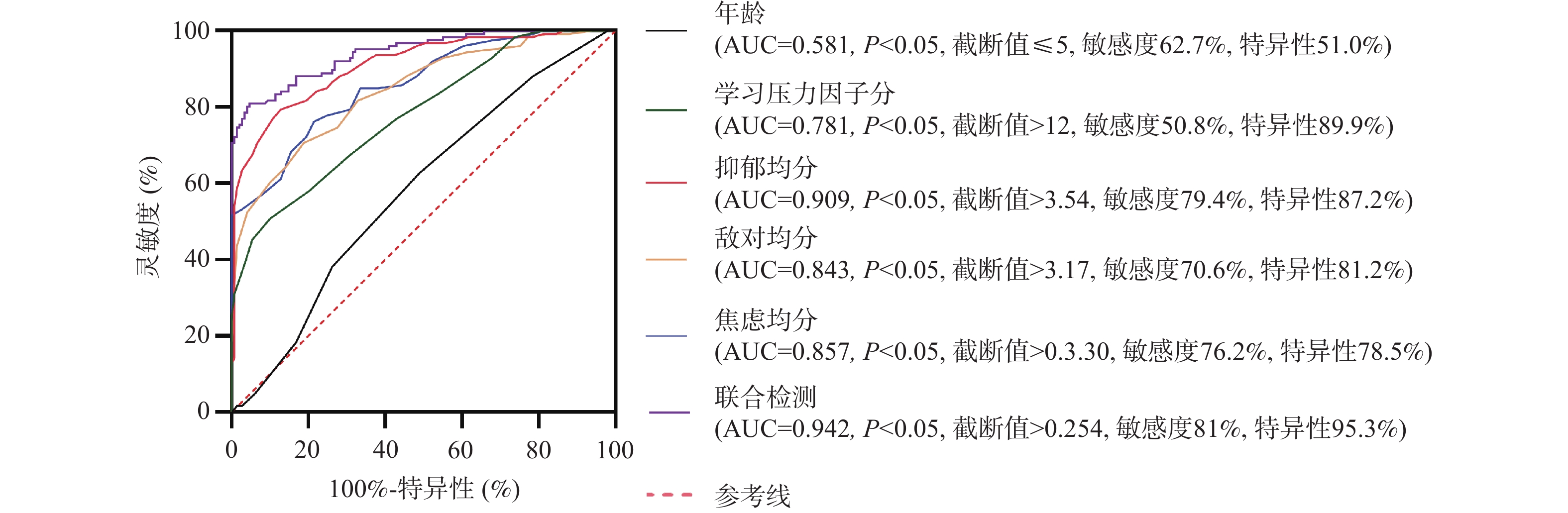
目的 探讨滇南某地区少数民族聚集地首发青少年抑郁症患者自杀意念的影响因素。 方法 纳入2023年3月至2024年7月期间,因情绪低落主诉于玉溪市人民医院及墨江县人民医院精神科门诊就诊,且符合抑郁症诊断标准的首发青少年患者277例。将患者分为伴有自杀意念组(n = 128)和不伴有自杀意念组(n = 149)。采用症状自评量表(symptom checklist-90,SCL-90)、贝克焦虑量表(Beck anxiety inventory,BAI)、贝克抑郁量表(Beck depression inventory,BDI)、匹兹堡睡眠量表(Pittsburgh sleep quality index,PSQI)及青少年生活事件量表(adolescent self-rating life events checklist,ASLEC)评估心理因素。应用Logistic回归分析确定首发青少年抑郁症患者(总样本及女性亚组)自杀意念的独立预测因子。基于Logistic回归系数构建联合预测概率模型,通过绘制受试者工作特征(receiver operating characteristic,ROC)曲线评估单个因子和联合预测模型对自杀意念的预测效能。 结果 伴有自杀意念组的ASLEC总分、SCL-90总分及各因子得分,以及BAI总分、BDI总分、PSQI总分均高于不伴有自杀意念组,差异具有统计学意义(P均 < 0.01)。多因素Logistic回归分析显示,年龄、学习压力因子得分、抑郁因子得分、敌对因子得分及焦虑因子得分是首发青少年抑郁症患者自杀意念的独立预测因子。对于女性首发青少年抑郁症患者,年龄及SCL-90总均分是其自杀意念的独立预测因子。ROC曲线分析表明,年龄、学习压力因子得分、抑郁因子得分、敌对因子得分、焦虑因子得分及组合均对首发青少年抑郁症患者自杀意念具有显著的预测价值(P < 0.05),其中组合预测价值效能最高(AUC = 0.942);在女性首发青少年抑郁症患者中,年龄、SCL-90总均分及组合对自杀意念亦具有较高预测价值(均P < 0.05),组合预测因子效能同样最高(AUC = 0.758)。 结论 年龄较小、学习压力、抑郁、敌对及焦虑因子分是首发青少年抑郁症患者自杀意念的独立预测因子,联合预测效能显著优于单一因子;年龄较小及SCL-90总症状严重程度是女性患者的特异性独立预测因子。 Abstract:Objective To explore the influencing factors of suicidal ideation in first-episode adolescent patients with depression in an ethnic minority concentrated area in southern Yunnan. Methods A total of 277 first-episode adolescent patients who presented to the psychiatric outpatient departments of Yuxi City People’ s Hospital and Mojiang County People’ s Hospital between March 2023 and July 2024 with chief complaints of depressed mood and met diagnostic criteria for depression were enrolled. Patients were divided into two groups: those with suicidal ideation (n = 128) and those without suicidal ideation (n = 149). Psychological factors were evaluated using the Symptom Checklist-90 (SCL-90), Beck Bnxiety Inventory (BAI), Beck Depression Inventory (BDI), Pittsburgh Sleep Quality Index (PSQI), and Adolescent Self-Rating Life Events Checklist (ASLEC). Logistic regression analysis was applied to determine independent predictive factors of suicidal ideation in first-episode adolescent depression patients (total sample and female subgroup). A combined predictive probability model was constructed based on Logistic regression coefficients, and the predictive efficacy of individual factors and the combined model for suicidal ideation was assessed by plotting Receiver Operating Characteristic (ROC) curves. Results The ASLEC total score, SCL-90 total score and subscale scores, BAI total score, BDI total score, and PSQI total score in the group with suicidal ideation were significantly higher than those in the group without suicidal ideation (P < 0.01). Multivariate logistic regression analysis showed that age, academic pressure subscale score, depression subscale score, hostility subscale score, and anxiety subscale score were independent predictive factors of suicidal ideation in first-episode adolescent depression patients. For female first-episode adolescent depression patients, age and SCL-90 mean total score were independent predictive factors of suicidal ideation. ROC curve analysis indicated that age, academic pressure subscale score, depression subscale score, hostility subscale score, anxiety subscale score, and their combination all had significant predictive value for suicidal ideation in first-episode adolescent depression patients (P < 0.05), with the combined model showing the highest predictive efficacy (AUC = 0.942). In female first-episode adolescent depression patients, age, SCL-90 mean total score, and their combination also had high predictive value for suicidal ideation (P < 0.05), with the combined predictive model similarly demonstrating the highest efficacyas well (AUC = 0.758). Conclusion The independent predictors of suicidal ideation in first-episode adolescent depression patients are younger age, learning pressure, depression, hostility and anxiety factor scores. The combined pr edictive efficacy is significantly better than that of a single factor. Younger age and the total symptom severity of SCL -90 are the specific independent predictors for female patients. -
Key words:
- Adolescent depression /
- Suicidal ideation /
- Adolescent life events /
- Symptom checklist-90
-
表 1 两组抑郁症患者的一般资料[($\bar x \pm s $)/n(%)]
Table 1. General information of the two groups of depression patients [($\bar x \pm s $)/n(%)]
项目 不伴有自杀意念组(n = 149) 伴有自杀意念组(n = 128) χ2/t P 年龄(岁) 15.26 ± 1.73 14.86 ± 1.52 2.041 0.042* 性别 14.492 < 0.001* 男 103(46.0) 112(43.8) 女 46(30.9) 46(12.5) *P < 0.05。 表 2 男性组与女性组抑郁患者的量表得分比较[n(%)/M(P25,P75)]/($\bar x \pm s $)]
Table 2. Comparison of scale scores between male and female depression patients [n(%)/M(P25,P75)/($ \bar x \pm s $)]
项目 男性(n = 61) 女性(n = 216) X2/Z/t P 年龄(岁) 16.0(14.5,17.0) 15.0(14.0,16.0) −2.503 0.012* ASLE评分 总分 37.0(20.0,56.0) 48.5(35.0,70.0) −3.762 < 0.001* 人际关系因子分 10.0(4.25,15.00) 15.0(10.0,20.00) −4.540 < 0.001* 学习压力因子分 8.00(4.50,11.75) 11.00(8.00,14.00) −3.589 0.001* 受惩罚因子分 7.02 ± 5.68 8.62 ± 6.38 −1.763 0.256 丧失因子分 3.03 ± 3.90 3.77 ± 3.72 −1.345 0.738 健康适应因子分 4.75 ± 3.54 6.39 ± 3.73 −3.035 0.795 其他方面分 6.00(3.00,9.75) 8.00(5.00,11.00) −2.979 0.003* 匹兹堡总分 10.00(6.00,13.00) 12.00(9.00,14.00) −2.785 0.005* 焦虑标准总分 53.50(38.25,66.75) 66.00(54.00,78.00) −4.591 < 0.001* 抑郁总分 30.00(19.00,36.75) 38.00(30.00,46.00) −5.045 < 0.001* SCL-90 总分 24.56(20.49,28.71) 30.61(26.58,37.14) −5.785 < 0.001* 躯体化均分 2.21(1.60,2.81) 2.83(2.33,3.42) −5.037 < 0.001* 强迫症状均分 2.60(1.90,3.10) 3.20(2.60,3.70) −4.797 < 0.001* 人际关系均分 2.50(1.89,3.30) 3.33(2.56,3.78) −4.799 < 0.001* 抑郁均分 2.65(1.94,3.54) 3.62(2.77,4.23) −4.687 < 0.001* 焦虑均分 2.55(2.20,3.37) 3.40(2.70,4.00) −4.925 < 0.001* 敌对均分 2.33(1.67,3.17) 3.17(2.50,3.83) −5.327 < 0.001* 恐怖均分 2.00(1.43,2.67) 2.86(2.14,3.71) −5.295 < 0.001* 偏执均分 2.50(1.67,3.33) 3.00(2.33,3.50) −3.104 < 0.001* 精神病性均分 2.55(1.92,3.20) 3.10(2.40,3.60) −3.180 < 0.001* 其他均分 2.71(1.89,3.29) 3.29(2.71,3.86) −4.602 < 0.001* *P < 0.05。 表 3 2组抑郁症患者的一般情况及量表得分比较[n(%)/M(P25,P75)/($\bar x \pm s $)]
Table 3. Comparison of general conditions and scale scores of the two groups of depression patients [n(%)/M(P25,P75)/($\bar x \pm s $)]
项目 不伴有自杀意念组(n = 149) 伴有自杀意念组(n = 128) Z P 性别(男) 103(46) 112(14) 14.492b < 0.001* ASLEC评分 总分 37.0(24.50,50.50) 58.00(46.75,77.25) −8.855c < 0.001* 人际关系因子分 11.00(6.00,15.50) 17.00(11.75,21.00) −6.566c < 0.001* 学习压力因子分 9.00(6.00,11.00) 13.00(10.00,17.00) −8.047c < 0.001* 受惩罚因子分 5.00(2.00,9.00) 10.00(6.00,16.00) −6.724c < 0.001* 丧失因子分 2.00(0.00,4.00) 5.00(2.00,8.00) −6.030c < 0.001* 健康适应因子分 4.00(2.00,7.00) 7.50(5.00,10.00) −6.089c < 0.001* 其他方面分 6.00(3.00,8.00) 9.00(7.00,13.00) −7.773c < 0.001* 匹兹堡总分 10.00(6.50,12.00) 13.00(11.00,15.25) −7.485c < 0.001* 焦虑标准总分 57.00(42.00,65.00) 76.50(64.75,83.00) −9.569c < 0.001* 抑郁总分 30.00(21.50,36.50) 43.50(37.00,48.00) −10.103c < 0.001* SCL-90 总分 25.97(22.11,28.65) 36.44(31.53,39.27) −11.794c < 0.001* 躯体化均分 2.33(1.75,2.75) 3.25(2.73,3.75) −9.303c < 0.001* 强迫症状均分 2.60(2.15,3.10) 3.70(3.10,4.00) −9.857c < 0.001* 人际关系均分 2.56(2.00,3.22) 3.67(3.30,4.11) −10.038c < 0.001* 抑郁均分 2.69(1.88,3.34) 4.08(3.69,4.46) −11.697c < 0.001* 焦虑均分 2.70(2.25,3.25) 4.00(3.40,4.30) −10.217c < 0.001* 敌对均分 2.50(1.91,3.17) 3.83(3.00,4.33) −9.813c < 0.001* 恐怖均分 2.14(1.50,2.78) 3.43(2.71,4.00) −9.574c < 0.001* 偏执均分 2.50(2.00,3.08) 3.41(2.83,4.00) −8.046c < 0.001* 精神病性均分 2.50(1.90,3.10) 3.40(2.90,3.82) −8.165c < 0.001* 其他均分 2.71(2.14,3.29) 3.71(3.29,4.00) −8.869c < 0.001* 注:b代表x2值,c代表z值。 表 4 抑郁症患者伴自杀意念的独立危险因素分析
Table 4. Analysis of independent risk factors for suicidal ideation in depression patients
因变量 回归系数 标准误 χ2 OR 95%CI P 年龄 −0.313 0.131 5.717 0.731 0.565~0.945 0.017* 学习压力因子分 0.255 0.072 12.619 1.291 1.121~1.486 < 0.001* 抑郁均分 1.390 0.301 21.332 4.014 2.226~7.239 < 0.001* 焦虑均分 0.795 0.352 5.086 2.214 1.110~4.418 0.024* 敌对均分 1.023 0.282 13.186 2.782 1.601~4.833 < 0.001* 常量 −8.530 2.254 14.323 0.000 < 0.001* 注:以出现自杀意念为因变量(是 = 1,否 = 0);OR≥1表示该因素是自杀意念的危险因素;*P < 0.05。 表 5 女性抑郁症患者自杀意念形成的独立影响因素分析
Table 5. Analysis of independent influencing factors for the formation of suicidal intentions in female depression patients
因变量 回归系数 标准误 χ2 OR 95%CI P 年龄 −0.222 0.096 5.371 0.801 0.664~0.966 0.020* SCL-90 0.136 0.025 28.890 1.146 1.090~1.204 < 0.001* 常量 0.837 1.533 0.298 2.310 0.585 OR≥1表示该因素是自杀意念的危险因素;*P < 0.05。 -
[1] Melhem N M, Porta G, Oquendo M A, et al. Severity and variability of depression symptoms predicting suicide attempt in high-risk individuals[J]. JAMA Psychiatry, 2019, 76(6): 603-613. doi: 10.1001/jamapsychiatry.2018.4513 [2] Serra G, De Crescenzo F, Maisto F, et al. Suicidal behavior in juvenile bipolar disorder and major depressive disorder patients: Systematic review and meta-analysis[J]. J Affect Disord, 2022, 311: 572-581. doi: 10.1016/j.jad.2022.05.063 [3] Barbeito S, Vega P, Sánchez-Gutiérrez T, et al. A systematic review of suicide and suicide attempts in adolescents with psychotic disorders[J]. Schizophr Res, 2021, 235: 80-90. doi: 10.1016/j.schres.2021.07.029 [4] Liu D, Liu S, Deng H, et al. Depression and suicide attempts in Chinese adolescents with mood disorders: The mediating role of rumination[J]. Eur Arch Psychiatry Clin Neurosci, 2023, 273(4): 931-940. doi: 10.1007/s00406-022-01444-2 [5] Bostwick J M, Pankratz V S. Affective disorders and suicide risk: A reexamination[J]. Am J Psychiatry, 2000, 157(12): 1925-1932. doi: 10.1176/appi.ajp.157.12.1925 [6] 梁军林, 孙录, 赵静波, 等. 中学生自杀意念发生率及其影响因素分析[J]. 临床精神医学杂志, 2000, 10(3): 144-146. [7] Choquet M, Menke H. Suicidal thoughts during early adolescence: Prevalence, associated troubles and help-seeking behavior[J]. Acta Psychiatr Scand, 1990, 81(2): 170-177. [8] Miranda R, Ortin A, Scott M, et al. Characteristics of suicidal ideation that predict the transition to future suicide attempts in adolescents[J]. J Child Psychol Psychiatry, 2014, 55(11): 1288-1296. doi: 10.1111/jcpp.12245 [9] ChanL F, Shamsul A S, Maniam T. Are predictors of future suicide attemptsand the transition from suicidal ideation to suicide attempts shared or distinct: A 12-month prospective study among patients with depressive disorders[J]. Psychiatry Res, 2014, 220(3): 867-873. doi: 10.1016/j.psychres.2014.08.055 [10] Duarte T A, Paulino S, Almeida C, etal. Self-harm as a predisposition for suicide attempts: A study of adolescents' deliberate self-harm, suicidal ideation, and suicide attempts[J]. Psychiatry Res, 2020, 287: 112553. doi: 10.1016/j.psychres.2019.112553 [11] Li Y, Li P, Yuan M, et al. Social-ecological perspective on the suicidal behaviour factors of early adolescents in China: A network analysis[J]. Gen Psychiatr, 2024, 37(1): e101317. doi: 10.1136/gpsych-2023-101317 [12] Healy D. Lines of evidence on the risks of suicide with selective serotonin reuptake inhibitors[J]. Psychother Psychosom, 2003, 72(2): 71-79. doi: 10.1159/000068691 [13] Nock M K, Borges G, Bromet E J. Prevalence and risk factors for suicidal ideation, plans and attempts[J]. British Journal of Psychiatry, 2008, 192(2): 98-105. doi: 10.1001/jamapsychiatry.2018.4513 [14] Wang L, Cheng H, Qu Y, et al. The prevalence of child maltreatment among Chinese primary and middle school students: A systematic review and meta-analysis[J]. Soc Psychiatry Psychiatr Epidemiol, 2020, 55(9): 1105-1119. doi: 10.1007/s00127-020-01916-7 [15] Tillery R, Willard V W, Howard SharpK M, et al. Impact of the parent-child relationship on psychological and social resilience in pediatric cancer patients[J]. Psychooncology, 2020, 29(2): 339-346. doi: 10.1002/pon.5258 [16] Nadorff M R, Nazem S, Fiske A. Insomnia symptoms, nightmares, and suicide risk: Duration of sleep disturbance matters[J]. Suicide Life Threat Behav, 2013, 43(2): 139-149. doi: 10.1111/sltb.12003 [17] Liu X, Tein J Y. Life events, psychopathology, and suicidal behavior in Chinese adolescents[J]. JAffectDisord, 2005, 86(2-3): 195-203. doi: 10.1016/j.jad.2005.01.016 [18] World Health Organization. The ICD-10 classification of mental and behavioural disorders: diagnostic criteria for research[EB/OL]. (1993-01-01)[2023-06-01]. https://www.who.int/Publications/i/item/9241544554. [19] 刘贤臣, 刘连启, 杨杰, 等. 青少年生活事件量表的信度效度检验[J]. 中国临床心理学杂志, 1997, 5(1): 34-36. doi: 10.13342/j.cnki.cjhp.2021.05.015 [20] 汪向东, 王希林, 马弘. 心理卫生评定量表手册[K]. 中国心理卫生杂志社, 1999. [21] 朱智贤. 心理学大词典[M]. 北京: 北京师范大学出版社, 1989: 110. [22] Vella E J, Kamarck T W, Flory J D, et al. Hostile mood and social strain during daily life: A test of the transactional model[J]. Ann Behav Med, 2012, 44(3): 341-352. doi: 10.1007/s12160-012-9400-7 [23] Kessler R C, McGonagle K A, Zhao S, et al. Lifetime and 12-month prevalence of DSM-III-R psychiatric disorders in the United States. Results from the National Comorbidity Survey[J]. Arch Gen Psychiatry, 1994, 51(1): 8-19. doi: 10.1001/archpsyc.1994.03950010008002 [24] Kessler R C, Chiu W T, Demler O, et al. Prevalence, severity, and comorbidity of 12-month DSM-IV disorders in the National Comorbidity Survey Replication[J]. Arch Gen Psychiatry, 2005, 62(6): 617-627. [25] Marcus S M, Kerber K B, Rush A J, et al. Sex differences in depression symptoms in treatment-seeking adults: Confirmatory analyses from the Sequenced Treatment Alternatives to Relieve Depression study[J]. Compr Psychiatry, 2008, 49(3): 238-246. doi: 10.1016/j.comppsych.2007.06.012 [26] Schuch J J J, Roest A M, Nolen W A, et al. Gender differences in major depressive disorder: Results from the Netherlands study of depression and anxiety[J]. J Affect Disord, 2014, 156: 156-163. doi: 10.1016/j.jad.2013.12.011 [27] Gifuni A J, Perret L C, Lacourse E, et al. Decision-making and cognitive control in adolescent suicidal behaviors: A qualitative systematic review of the literature[J]. Eur Child Adolesc Psychiatry, 2021, 30(12): 1839-1855. doi: 10.1007/s00787-020-01550-3 [28] 高媛媛, 王冉, 任若佳, 等. 负性生活事件及心理弹性对青少年抑郁症患者自杀行为的影响[J]. 神经疾病与精神卫生, 2024, 24(9): 629-634. doi: 10.3969/j.issn.1009-6574.2024.09.004 [29] Thapar A, Eyre O, Patel V, et al. Depression in young people[J]. Lancet, 2022, 400(10352): 617-631. doi: 10.1016/S0140-6736(22)01012-1 [30] 徐莉, 赵锦涵, 金于雄, 等. 青少年抑郁症患者非自杀性自伤的相关因素[J]. 昆明医科大学学报, 2022, 43(5): 58-64. doi: 10.3969/j.issn.1009-6574.2024.10.004 [31] Fund United Nations Children’ s. The State of the World’ s Children 2021: On my mind promoting, protecting and caring for children’ s mentalhealth[M]. United Nations, 2021. -






 下载:
下载: