The Relationship Between Serum CTRP7 and CTRP15 Levels and Insulin Resistance and Maternal and Neonatal Outcomes in Patients with Gestational Diabetes Mellitus
-
摘要:
目的 探讨妊娠糖尿病患者血清C1q/肿瘤坏死因子相关蛋白7(complement c1q/tnf related proteins7,CTRP7)和CTRP15水平与胰岛素抵抗及母婴结局的关系。 方法 选取2023年1月至2024年5月入同济大学附属妇产科医院诊断为妊娠糖尿病患者139例为妊娠糖尿病组,根据母婴结局分为GDM结局正常组(n = 91)和GDM结局不良组(n = 48),另选取同期孕检健康孕妇100例为健康孕妇组。采用酶联免疫吸附试验(enzyme-linked immunosorbent assay,ELISA)法检测血清CTRP7和CTRP15水平,Pearson相关分析血清CTRP7、 CTRP15水平与胰岛素抵抗及血糖、血脂的相关性,Logistic回归分析母婴不良结局因素。 结果 娠糖尿病组孕期体重增加、胎盘重量、绒毛膜炎占比、HOMA-IR、FBG、TG、TC、LDL-C、FPG、FINS、HbAlc水平明显高于健康孕妇组, 健康膳食占比、运动占比、HOMA-β低于健康孕妇组(P < 0.05);妊娠糖尿病组患者血清CTRP7和CTRP15水平明显高于健康孕妇组(P < 0.05);血清CTRP7和CTRP15水平与HOMA-IR、FBG、TG、TC、LDL-C、FPG、FINS和HbAlc呈正相关性(P < 0.05),与HOMA-β呈负相关性(P < 0.05);GDM结局不良组孕期体重增加、绒毛膜炎占比、HOMA-IR、FBG、TG、TC、LDL-C、FPG、FINS、HbAlc水平显著高于GDM结局正常组,HOMA-β显著低于GDM结局正常组(P < 0.05)。孕期体重增加、绒毛膜炎、HOMA-IR、HOMA-β、FBG、TG、TC、LDL-C、FPG、FINS、HbAlc、CTRP7和CTRP15均是妊娠糖尿病患者母婴不良结局的影响因素(P < 0.05),三者联合预测价值明显高于三者单独检测(Z = 4.265、3.612、3.954,P < 0.001)。 结论 妊娠糖尿病患者血清中CTRP7和CTRP15水平明显升高,且与胰岛素抵抗密切相关,与HOMA-IR联合检测对不良母婴结局具有一定预测价值。 Abstract:Objective To investigate the relationship between serum C1q/tumor necrosis factor-related protein 7 (complement c1q/tnf related proteins7, CTRP7) and CTRP15 levels and insulin resistance (Insulin resistance) as well as maternal and neonatal outcomes in patients with gestational diabetes mellitus. Methods A total of 139 patients diagnosed with gestational diabetes at the Obstetrics and Gynecology Hospital Affiliated to Tongji University from January 2023 to May 2024 were selected as the gestational diabetes group. Based on maternal and neonatal outcomes, they were divided into a GDM with normal outcomes group (91 cases) and a GDM with adverse outcomes group (48 cases). Additionally, 100 healthy pregnant women who underwent prenatal check-ups during the same period were selected as the healthy pregnant women group. The serum levels of CTRP7 and CTRP15 were measured using the enzyme-linked immunosorbent assay (ELISA) method. Pearson correlation analysis was used to analyze the correlation between serum CTRP7 and CTRP15 levels and insulin resistance, blood glucose, and blood lipids. Logistic regression analysis was used to analyze the factors associated with adverse maternal and neonatal outcomes. Results The GDM group had significantly higher levels of gestational weight gain, placental weight, proportion of chorioamnionitis, HOMA-IR, FBG, TG, TC, LDL-C, FPG, FINS, and HbA1c compared to the healthy pregnant women group, while the proportions of healthy diet and exercise, and HOMA-β were lower than those in the healthy pregnant women group (P < 0.05). The serum levels of CTRP7 and CTRP15 in the GDM group were significantly higher than those in the healthy pregnant women group(P < 0.05). Serum CTRP7 and CTRP15 levels were positively correlated with HOMA-IR, FBG, TG, TC, LDL-C, FPG, FINS, and HbA1c (P < 0.05), and negatively correlated with HOMA-β (P < 0.05). The GDM with adverse outcomes group had significantly higher levels of gestational weight gain, proportion of chorioamnionitis, HOMA-IR, FBG, TG, TC, LDL-C, FPG, FINS, and HbA1c compared to the GDM with normal outcomes group, while HOMA-β was significantly lower than that in the GDM with normal outcomes group (P<0.05). Maternal weight gain during pregnancy, chorioamnionitis, HOMA-IR, HOMA-β, FBG, TG, TC, LDL-C, FPG, FINS, HbAlc, CTRP7, and CTRP15 are all influencing factors for adverse maternal and neonatal outcomes in patients with gestational diabetes mellitus (P<0.05). The combined predictive value of the three is significantly higher than that of each alone (Z=4.265, 3.612, 3.954, P<0.001). Conclusion Serum levels of CTRP7 and CTRP15 are significantly elevated in patients with gestational diabetes mellitus (GDM) and are closely related to insulin resistance. Combined detection with HOMA-IR has certain predictive value for adverse maternal and infant outcomes. -
Key words:
- Gestational diabetes mellitus /
- CTRP7 /
- CTRP15 /
- Insulin resistance /
- Maternal and infant outcome
-
表 1 两组患者的临床资料对比分析[($\bar x\pm s $ )/n(%)]
Table 1. Comparative analysis of clinical data between the two groups of patients[( $\bar x\pm s $)/n(%)]
组别 健康孕妇组(n=100) 妊娠糖尿病组(n=139) t P 年龄(岁) 28.09 ± 4.19 29.11 ± 4.21 1.851 0.065 孕前 BMI(kg/m2) 21.52 ± 2.27 22.04 ± 2.34 1.716 0.087 增加 BMI(kg/m2) 3.56 ± 1.27 3.81 ± 1.32 1.461 0.143 孕周(周) 26.61 ± 2.23 26.84 ± 2.81 0.679 0.498 收缩压(mmHg) 110.56 ± 10.19 112.81 ± 10.24 1.679 0.094 舒张压(mmHg) 70.78 ± 5.64 72.04 ± 8.13 1.355 0.183 孕期体重增加(kg) 11.75 ± 5.16 13.89 ± 6.07 2.859 0.005* 膳食结构 高盐高油膳食 10(10.00) 35(25.18) 8.901 0.012* 高脂膳食 18(18.00) 23(16.55) 健康膳食 72(72.00) 81(58.27) 体力活动 运动 69(69.00) 74(53.24) 6.013 0.014* 不运动 31(31.00) 65(46.76) 胎盘重量(g) 510.29 ± 9.87 517.86 ± 11.32 5.376 < 0.001* 绒毛膜炎 0(0.00) 13(9.35) 9.89 0.002* HOMA-IR 2.34 ± 0.49 4.61 ± 1.08 19.608 < 0.001* FBG(mmol/L) 4.29 ± 0.97 6.50 ± 1.03 16.764 < 0.001* TG(mmol/L) 2.63 ± 0.73 3.82 ± 0.81 11.671 < 0.001* TC(mmol/L) 5.29 ± 0.78 6.48 ± 0.80 11.463 < 0.001* HDL-C(mmol/L) 1.64 ± 0.42 1.69 ± 0.46 0.859 0.391 LDL-C(mmol/L) 2.61 ± 0.56 3.17 ± 0.74 6.367 < 0.001* FPG(mmol/L) 4.68 ± 0.25 5.56 ± 0.37 20.63 < 0.001* FINS(mU/L) 12.82 ± 3.51 15.29 ± 3.42 5.447 < 0.001* HbAlc(%) 4.79 ± 0.57 5.94 ± 0.82 12.078 < 0.001* ALB(ng/ml) 38.28 ± 2.93 38.33 ± 2.97 0.129 0.897 Hb(g/L) 115.93 ± 15.18 117.42 ± 15.26 0.746 0.456 *P < 0.05。 表 2 两组患者血清CTRP7和CTRP15水平对比分析[( $\bar x\pm s $)/n(%)]
Table 2. Comparative analysis of serum CTRP7 and CTRP15 levels between the two patient groups[($\bar x\pm s $)/n(%)]
组别 n CTRP7(μg/L) CTRP15(μg/L) 健康孕妇组 100 109.58 ± 27.36 35.69 ± 9.45 妊娠糖尿病组 139 184.26 ± 31.42 73.21 ± 18.37 t 19.117* 18.713* P < 0.001 < 0.001 *P < 0.05。 表 3 血清CTRP7、CTRP15水平与血糖、血脂及胰岛素抵抗的关系
Table 3. Relationship between serum CTRP7 and CTRP15 levels with blood glucose,blood lipids,and insulin resistance
指标 CTRP7 CTRP15 r P r P HOMA-IR 0.475 < 0.001* 0.492 < 0.001* FBG 0.319 < 0.001* 0.325 < 0.001* TG 0.392 < 0.001* 0.403 < 0.001* TC 0.407 < 0.001* 0.418 < 0.001* LDL-C 0.519 < 0.001* 0.426 < 0.001* FPG 0.391 < 0.001* 0.381 < 0.001* FINS 0.474 < 0.001* 0.417 < 0.001* HbAlc 0.501 < 0.001* 0.434 < 0.001* *P < 0.05。 表 4 不同母婴结局患者临床资料对比分析[($\bar x\pm s $)/n(%)]
Table 4. Comparative analysis of clinical data among patients with different maternal-infant outcomes[($\bar x\pm s $)/n(%)]
组别 GDM结局正常组(n=91) GDM结局不良组(n=48) t P 年龄(岁) 28.75 ± 4.16 29.64 ± 4.25 1.19 0.236 孕前 BMI(kg/m2) 21.72 ± 2.29 22.37 ± 2.38 1.569 0.119 增加 BMI(kg/m2) 3.65 ± 1.28 3.83 ± 1.36 0.735 0.464 孕周(周) 26.73 ± 2.41 26.95 ± 2.92 0.475 0.636 收缩压(mmHg) 112.75 ± 9.47 114.93 ± 8.02 1.358 0.177 舒张压(mmHg) 71.49 ± 6.73 72.21 ± 8.57 0.544 0.587 孕期体重增加(kg) 12.29 ± 5.18 14.63 ± 6.26 2.353 0.020* 膳食结构 高盐高油膳食 21(23.08) 14(29.17) 0.676 0.713 高脂膳食 15(16.48) 8(16.67) 健康膳食 55(60.44) 26(54.17) 体力活动 运动 51(56.04) 23(47.92) 0.834 0.361 不运动 40(43.96) 25(52.08) 胎盘重量(g) 516.27 ± 10.98 519.35 ± 11.49 1.549 0.124 绒毛膜炎 5(5.49) 8(16.67) 4.627 0.031* HOMA-IR 3.79 ± 0.84 5.72 ± 1.25 10.821 < 0.001* FBG(mmol/L) 5.22 ± 0.99 6.76 ± 1.18 8.152 < 0.001* TG(mmol/L) 2.92 ± 0.79 4.18 ± 0.92 8.44 < 0.001* TC(mmol/L) 5.73 ± 0.75 6.96 ± 0.89 8.61 < 0.001* HDL-C(mmol/L) 1.66 ± 0.44 1.71 ± 0.49 0.612 0.541 LDL-C(mmol/L) 2.78 ± 0.61 3.39 ± 0.82 4.961 < 0.001* FPG(mmol/L) 4.73 ± 0.29 5.94 ± 0.45 19.207 < 0.001* FINS(mU/L) 13.72 ± 3.27 16.84 ± 3.62 5.153 < 0.001* HbAlc(%) 4.92 ± 0.59 6.24 ± 0.91 10.333 < 0.001* ALB(ng/ml) 38.31 ± 2.94 38.35 ± 3.01 0.076 0.939 Hb(g/L) 115.99 ± 15.20 117.83 ± 15.32 0.677 0.499 *P < 0.05。 表 5 不同母婴结局患者血清CTRP7、 CTRP15水平对比分析($\bar x\pm s $ )
Table 5. Comparative analysis of serum CTRP7 and CTRP15 levels in patients with different maternal-infant outcomes( $\bar x\pm s $)
组别 n CTRP7(μg/L) CTRP15(μg/L) GDM 结局正常组 91 123.84 ± 28.47 47.84 ± 12.43 GDM 结局不良组 48 192.18 ± 32.39 82.67 ± 20.55 t 12.824* 12.439* P < 0.001 < 0.001 *P < 0.05。 表 6 Logistic回归分析母婴不良妊娠结局因素
Table 6. Logistic regression analysis of factors associated with adverse maternal and fetal pregnancy outcomes
因素 β SE Wald χ2 P OR 95%CI 孕期体重增加 1.046 0.319 9.469 0.001* 2.846 1.523-5.318 绒毛膜炎 1.217 0.347 9.697 0.001* 3.377 1.710-6.666 HOMA-IR 1.034 0.321 9.411 0.002* 2.812 1.499-5.275 FBG 0.871 0.219 10.167 < 0.001* 2.389 1.555-3.670 TG 1.164 0.382 9.237 0.003* 3.203 1.514-6.771 TC 1.627 0.231 13.233 < 0.001* 5.089 3.235-8.002 LDL-C 1.521 0.396 10.031 < 0.001* 4.577 2.106-9.945 FPG 0.853 0.327 8.799 0.010* 2.347 1.236-4.454 FINS 1.436 0.316 10.734 < 0.001* 4.204 2.262-7.809 HbAlc 0.791 0.332 8.573 0.019* 2.206 1.150-4.227 CTRP7 1.384 0.216 12.597 < 0.001* 3.991 2.613-6.094 CTRP15 1.075 0.278 10.057 < 0.001* 2.93 1.699-5.052 *P < 0.05。 表 7 HOMA-IR、CTRP7和CTRP15 单独及联合预测母婴结局的价值分析
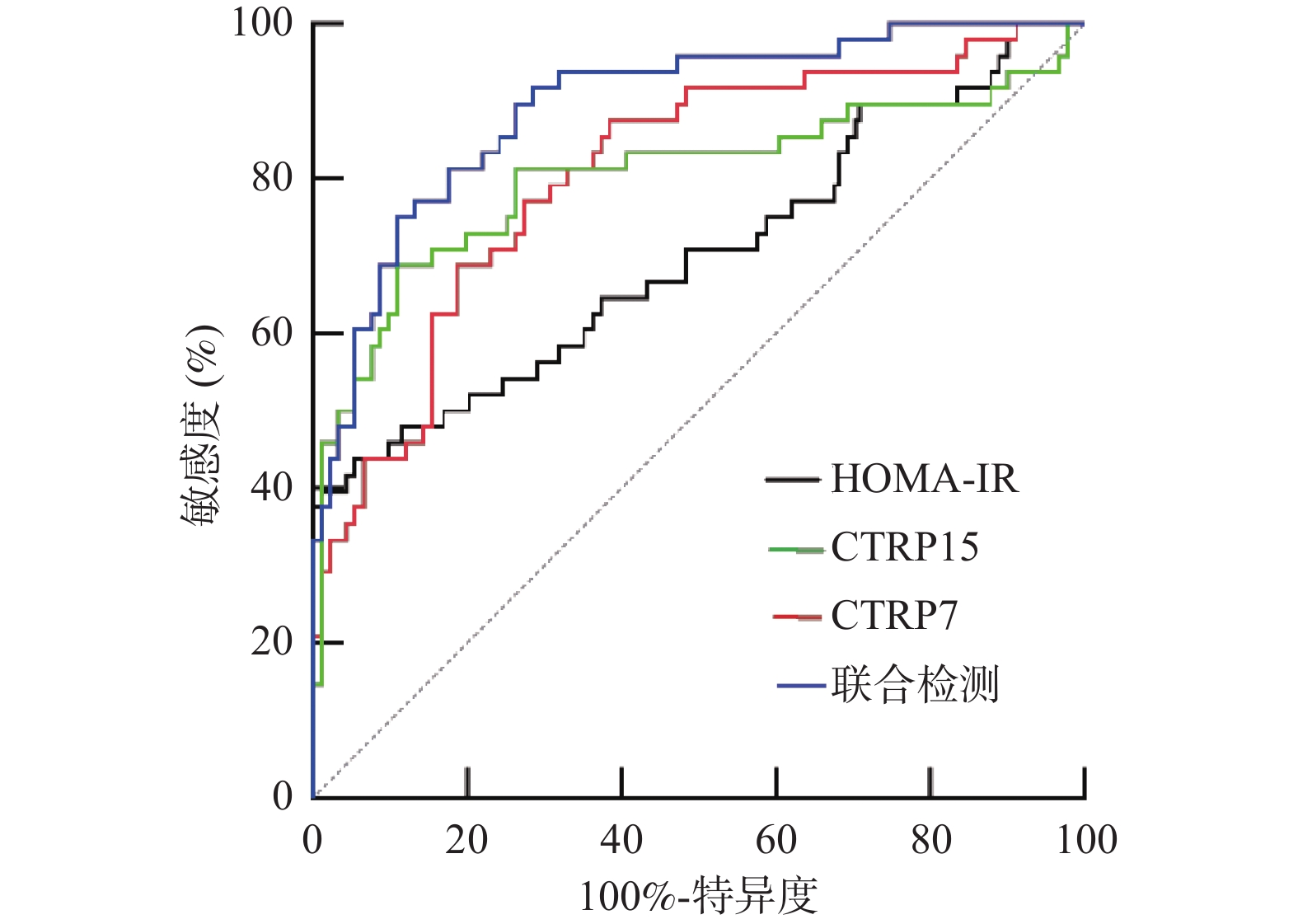
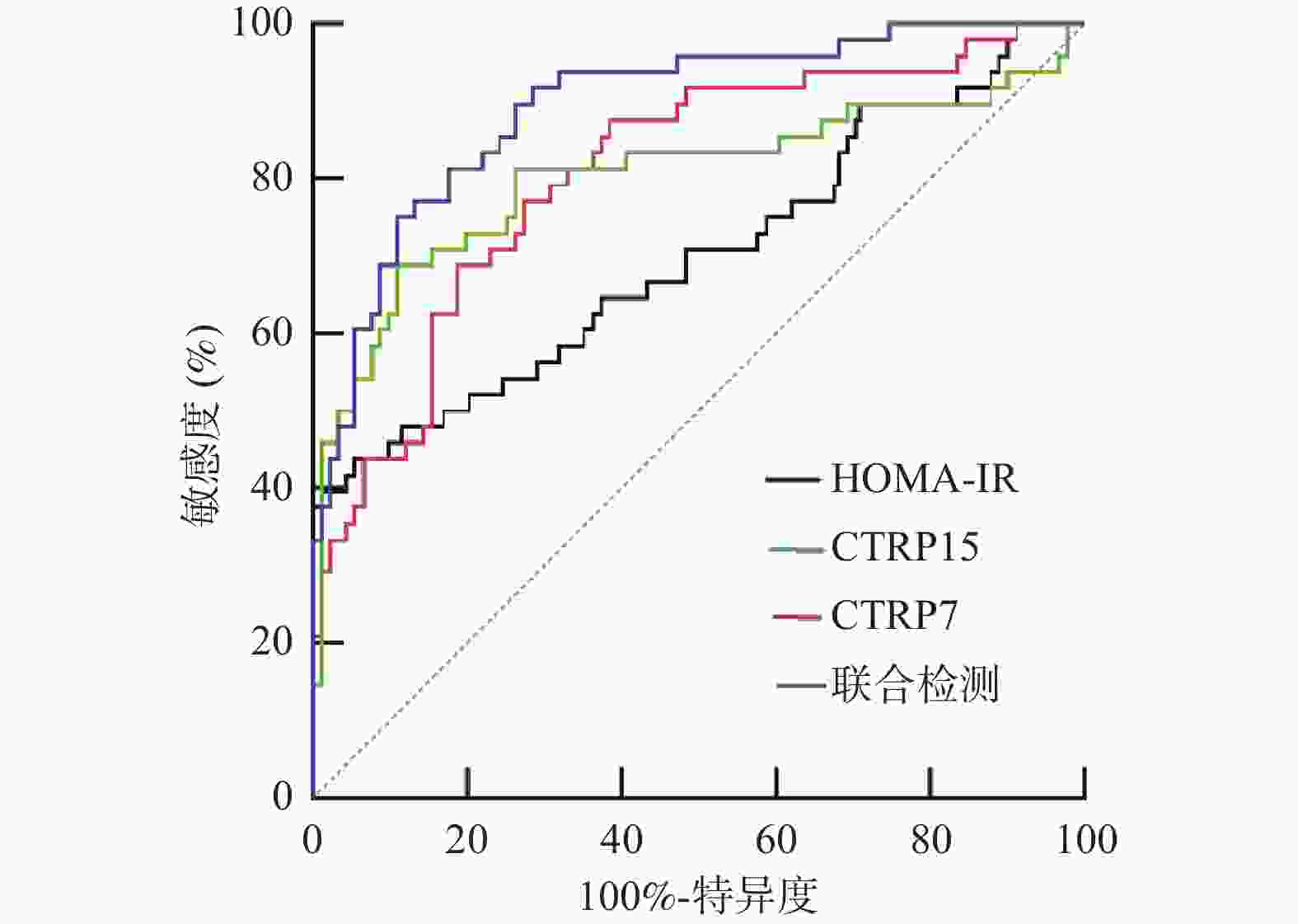
Table 7. Value analysis of HOMA-IR,CTRP7,and CTRP15 alone and in combination for predicting maternal and neonatal outcomes
预测项目 AUC值 95%CI 敏感度% 特异度% 约登指数 截断值 HOMA-IR 0.701 0.602-0.799 70.83 78.39 0.492 4.03 CTRP7 0.812 0.729-0.884 83.33 71.56 0.549 146.78 μg/L CTRP15 0.803 0.712-0.893 81.25 72.44 0.537 63.22 μg/L 联合检测 0.893 0.837-0.949 91.67 67.25 0.589 − -
[1] 瞿秀琴, 解双, 王尹梦, 等. 妊娠糖尿病患者血糖管理行为状况及影响因素分析[J]. 中国医药导报, 2024, 21(17): 35-38. [2] 张利玲, 安昱静, 张肖, 等. 妊娠糖尿病患者血清LRG1和CCL2水平对产后血糖转归的预测价值[J]. 临床和实验医学杂志, 2024, 23(11): 1192-1196. [3] 叶青燕, 吴凯, 练华珍. 孕期增长体质量、脂代谢指标与妊娠糖尿病患者不良妊娠结局的关系[J]. 检验医学与临床, 2024, 21(11): 1622-1626. [4] 邢慧敏, 田美玲, 云聪, 等. 不同时期应用双歧杆菌三联活菌胶囊治疗妊娠糖尿病对患者肠道微生态及妊娠结局的影响[J]. 川北医学院学报, 2024, 39(4): 532-537. [5] 王名岫, 黄悦, 崔鲂. 血清CTRP9、AMH对多囊卵巢综合征患者IVF-ET助孕结局的预测价值[J]. 中国卫生标准管理, 2024, 15(9): 36-40. [6] 童梦霞. 血清CTRP3、CTRP15水平与多囊卵巢综合征患者胰岛素抵抗的相关性研究[D]. 遵义: 遵义医科大学, 2021. [7] 杨卡明, 毕长龙. 肌联素与糖尿病胰岛素抵抗关系的研究进展[J]. 老年医学研究, 2024, 5(2): 47-51. doi: 10.3969/j.issn.2096-9058.2024.02.010 [8] 崔爽, 陈海英, 夏春玲. 妊娠糖尿病患者血清CTRP9水平与胰岛素抵抗的相关性[J]. 中国医科大学学报, 2025, 54(10): 954-957. [9] 中华医学会妇产科分会产科学组. 妊娠糖尿病的诊断标准[J]. 实用糖尿病杂志, 2009, 5(5): 62. [10] 王改华, 叶小琳. 妊娠糖尿病患者血清TXNIP、C-P水平对胎儿生长受限的预测价值[J]. 中国现代医学杂志, 2025, 35(13): 1-5. doi: 10.3969/j.issn.1005-8982.2025.13.001 [11] 王红红, 骆硕, 董巍巍, 等. 妊娠糖尿病IADPSG新诊断标准与母婴结局分析[J]. 国际检验医学杂志, 2019, 40(18): 2205-2208. [12] 朱毛根, 于康军, 牛三强. 妊娠糖尿病孕妇血清谷胱甘肽过氧化物酶3、水通道蛋白9表达水平及意义[J]. 实用临床医药杂志, 2024, 28(20): 86-91. doi: 10.7619/jcmp.20242347 [13] 蒋晓阳, 陈海霞, 曾紫伊. 多囊卵巢综合征患者发生妊娠期糖尿病的危险因素及胰岛素抵抗血脂水平对妊娠期糖尿病的预测价值[J]. 中国妇幼保健, 2025, 40(1): 62-65. [14] 蒋晶晶, 孙逸冕, 程丽. 妊娠期糖尿病孕妇孕前体重指数及孕中期糖化血清蛋白水平与大于胎龄儿关系及预测模型构建[J]. 陕西医学杂志, 2024, 53(7): 914-917. doi: 10.3969/j.issn.1000-7377.2024.07.010 [15] 陈丽, 卢国萍, 刘芙蓉. 血清Ghrelin、VEGF-A水平对妊娠期糖尿病患者早发型胎儿生长受限的预测价值[J]. 新疆医科大学学报, 2024, 47(5): 699-703. doi: 10.3969/j.issn.1009-5551.2024.05.014 [16] 吴佳娴, 王忆君, 张家怡, 等. 妊娠期糖尿病患者产后2年内发生2型糖尿病的影响因素及预测模型的构建[J]. 实用临床医药杂志, 2024, 28(16): 88-92, 97. [17] 徐玉红, 晋柏, 孙丽洲, 等. 妊娠期糖尿病孕妇胎盘和大网膜脂肪组织TNF-α及IL-1β的表达及其与胰岛素抵抗的关系[J]. 实用妇产科杂志, 2013, 29(10): 745-748. [18] 黄晶, 龙俊青. 基于孟德尔随机化分析研究儿童肥胖与妊娠期糖尿病的因果关系及性激素结合球蛋白的调节作用[J]. 现代妇产科进展, 2024, 33(3): 187-190. [19] Schanbacher C, Hermanns H M, Lorenz K, et al. Complement 1q/tumor necrosis factor-related proteins (CTRPs): Structure, receptors and signaling[J]. Biomedicines, 2023, 11(2): 559. [20] Xue S, Ling J, Tian M, et al. Combined serum CTRP7 and CTRP15 levels as a novel biomarker for insulin resistance and type 2 diabetes mellitus[J]. Heliyon, 2024, 10(9): e30029. doi: 10.1016/j.heliyon.2024.e30029 [21] 白家琪, 张林. 血清CTRP7水平与2型糖尿病相关性的研究进展[J]. 中国临床研究, 2025, 38(04): 629-632+637. doi: 10.13429/j.cnki.cjcr.2025.04.028 [22] Bi J, Duan Y, Wang M, et al. Deletion of large-conductance calcium-activated potassium channels promotes vascular remodelling through the CTRP7-mediated PI3K/Akt signaling pathway[J]. Acta Biochim Biophys Sin, 2022, 54(12): 1-11. doi: 10.3724/abbs.2022179 [23] Li K, Liang Z, Xu W, et al. CTRP7 is a biomarker related to insulin resistance and oxidative stress: Cross-sectional and intervention studies in vivo and in vitro[J]. Oxid Med Cell Longev, 2022, 2022: 6877609. doi: 10.1155/2022/6877609 [24] Ren M, Liu J, Zhang Y, et al. Retracted] effects of different ovulation induction regimens on sex hormone levels and serum CTRP3 and CTRP15 levels in patients with polycystic ovary syndrome (PCOS)[J]. BioMed Res Int, 2022, 2022: 6027878. doi: 10.1155/2022/6027878 [25] Ahmadi R, Fadaei R, Shokoohi Nahrkhalaji A, et al. The impacts of C1q/TNF-related protein-15 and adiponectin on Interleukin-6 and tumor necrosis factor-α in primary macrophages of patients with coronary artery diseases[J]. Cytokine, 2021, 142: 155470. doi: 10.1016/j.cyto.2021.155470 [26] Mohassel Azadi S, Shateri H, Mohammadi M, Fadaei R, et al. Increased circulating level of CTRP15 in patients with type 2 diabetes mellitus and its relation with inflammation and insulin resistance[J]. J Diabetes Metab Disord., 2021, 20(2): 1499-1504. doi: 10.1007/s40200-021-00892-2 [27] 桂琳, 董睿, 吴雪莲, 等. 补体C1q/肿瘤坏死因子相关蛋白家族在动脉粥样硬化中的作用[J]. 心血管病学进展, 2024, 45(6): 552-556. doi: 10.16806/j.cnki.issn.1004-3934.2024.06.017 [28] Shokoohi Nahrkhalaji A, Ahmadi R, Fadaei R, et al. Higher serum level of CTRP15 in patients with coronary artery disease is associated with disease severity, body mass index and insulin resistance[J]. Arch Physiol Biochem, 2022, 128(1): 276-280. doi: 10.1080/13813455.2019.1675713 [29] Fu J H, Huo J, Han Y M, et al. Predictive value of serum Gal-13, GLP-1 and VEGF levels in adverse pregnancy outcomes of gestational diabetes mellitus[J]. Zhonghua Yu Fang Yi Xue Za Zhi, 2023, 57(12): 2140-2146. -





 下载:
下载: